What is a migraine?
A migraine is a specific type of severe headache, usually affecting one side of the head, and accompanied by other symptoms such as nausea, vomiting, and sensitivity to light, sound, and smells.
- Prevalence: Migraine is a common neurological disorder affecting millions of people worldwide, with about
12% of the population affected. - Gender: Prevalence is higher in women (about 18%) than in men (about 6%).
- Age: Migraines usually begin in adolescence or early adulthood and may persist into middle age.

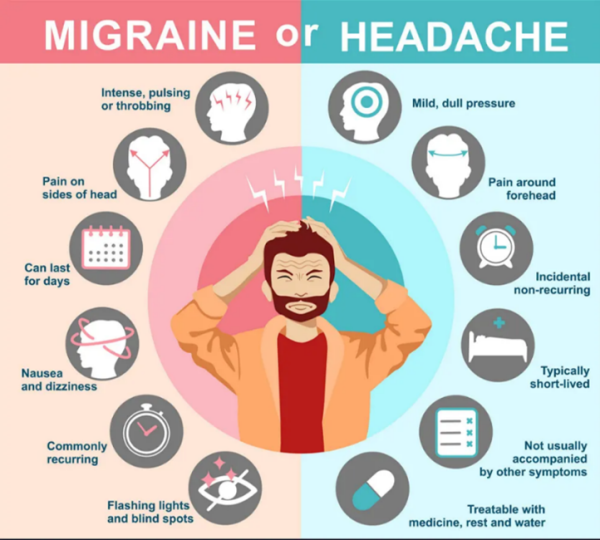
Differences between migraines and general headaches
General headaches, such as tension-type headaches or cluster headaches, are often milder, with a milder sense of pressure or tightness on both sides of the head, and without the neurological symptoms associated with migraines.
In short, migraine is a neurological disorder with complex symptoms, while headache itself is just a symptom.
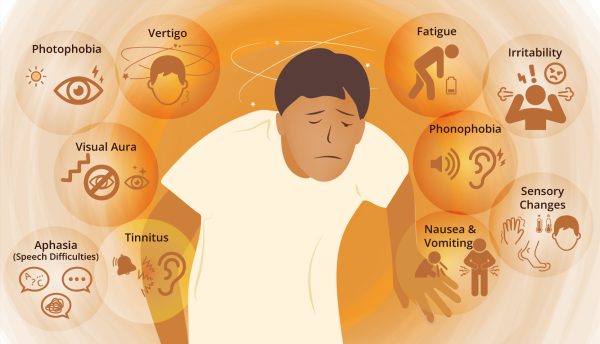
Common symptoms of migraine
- Severe, throbbing headache.
- Pain usually occurs on one side of the head, but it can also occur on both sides.
- Other accompanying symptoms include:
- Visual disturbances may occur before the headache starts, such as aura (flashes of light or blind spots).
- Dizziness or balance problems
- Often accompanied by gastrointestinal symptoms such as nausea and vomiting.
- Sensitivity to light, sound, and smells.
- Symptoms can last from hours to days.
- Symptoms can severely disrupt daily activities and affect quality of life.
Overuse and overdiagnosis of migraine
Strictly speaking, migraine is a truly debilitating neurological disorder, and its severe headaches can significantly affect quality of life.
Although migraines are common, overuse and overdiagnosis are also widespread, because the term is often used loosely to label many different types of headaches as migraines.
Reasons migraines are mislabeled include:
- The term is vague, and symptoms overlap with other types of headaches, such as tension-type headaches and cluster headaches.
- Misdiagnosis based on non-specific symptoms without a thorough evaluation.
Accurately diagnosing true migraine is crucial
- Accurately diagnosing true migraine based on established clinical criteria and appropriate specialist assessment is essential for headache patients to receive proper care, while also avoiding unnecessary medication for other types of headaches.
Pathophysiology of migraine
The theories and pathophysiological mechanisms related to migraine are quite complex and involve multiple factors, including genetics, environment, and neurobiology, as described below:
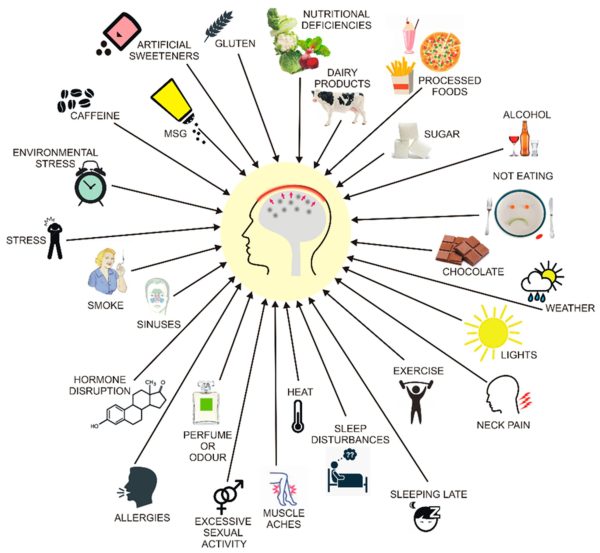
- Environmental triggers: Common migraine triggers include:
- Dietary factors: certain foods and drinks (alcohol, caffeine, chocolate, processed foods such as aged cheese)
- Environmental factors: bright light, irritating odors, weather changes
- Physical overexertion
- Stress and anxiety
- Sleep disturbances
- Hormonal changes: fluctuations in estrogen in women may affect serotonin regulation (e.g., during menstruation or pregnancy)
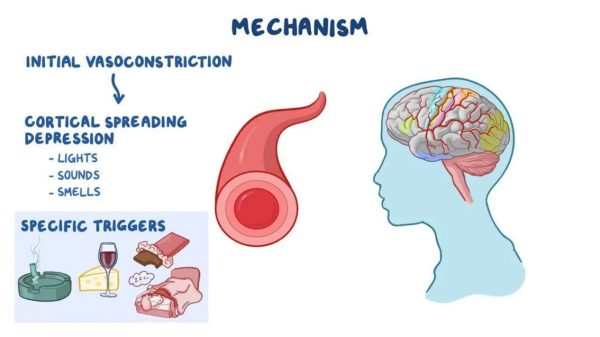
Neurovascular theory
- Cortical spreading depression (CSD): This phenomenon involves a wave of neuronal depolarization followed by a period of suppressed activity, which may lead to the aura symptoms experienced by some migraine sufferers.
- Vasodilation: After cortical spreading depression, inflammatory mediators are released, causing dilation of blood vessels in the brain. This vasodilation contributes to the onset of headache.
Neurotransmitter imbalance
- Serotonin (5-HT): Fluctuations in serotonin levels play an important role. Low serotonin levels may activate pain pathways in the brain.
- Calcitonin gene-related peptide (CGRP): Elevated CGRP levels are associated with migraine attacks. This neuropeptide promotes inflammation and vasodilation.
Genetic predisposition
- Familial association: Certain gene mutations have been shown to be linked to susceptibility to migraine, especially in cases of familial hemiplegic migraine.
- Interaction between genetic predisposition and environmental triggers: Genetic predisposition means migraine sufferers are born with a more sensitive nervous system, characterized by a lower threshold. This makes them more susceptible to environmental triggers such as stress, lack of sleep, hormonal changes, and dietary factors.
Psychological factors, central sensitization, and altered pain processing
- Altered pain processing: People with chronic migraine may experience central sensitization, along with certain psychological factors, making the nervous system more sensitive to pain signals and leading to heightened pain perception.
Assessment and investigations to confirm migraine
• Medical history: This includes reviewing the headache pattern, frequency, duration, triggers, associated symptoms, and overall neurological health.
• Neurological assessment: If the headache pattern or intensity changes suddenly, or if abnormal symptoms occur such as weakness, visual disturbances, or speech difficulties.
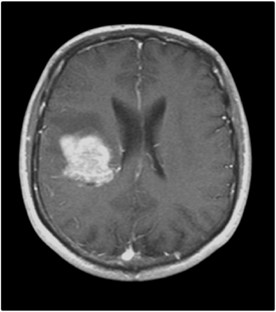
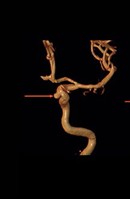
• Brain imaging: MRI (magnetic resonance imaging) can provide detailed brain images to rule out abnormalities such as tumors or aneurysms.
• Blood tests: To assess inflammation, infection, or metabolic disorders that may cause headaches
• Therefore, to accurately identify migraine, confirm the diagnosis, and develop an effective treatment plan, it is necessary to rule out other neurological disorders and other serious conditions through detailed investigations.
Treatments to reduce migraine frequency and severity:
• Acute medications: effectively relieve symptoms during a migraine attack
- Simple painkillers such as non-steroidal anti-inflammatory drugs (NSAIDs) (aspirin, ibuprofen, naproxen) can relieve mild symptoms by reducing inflammation and pain.
- Migraine-specific medications: triptans and ergot derivatives such as sumatriptan, rizatriptan, and zolmitriptan can relieve severe symptoms by constricting blood vessels and blocking pain pathways in the brain.
- Anti-nausea medications
• Migraine prevention measures:
- Identify and avoid triggers through lifestyle changes: By keeping a detailed migraine diary and analyzing patterns, migraines can be avoided through dietary adjustments, avoiding certain foods, and good sleep hygiene.
- Stress management: yoga, meditation, deep-breathing exercises
- Regular exercise: Consistent physical activity can reduce migraine attacks.
- Preventive treatment: Taking preventive medications for 4 to 8 weeks, such as beta-blockers, anti-seizure medications, antidepressants, botulinum toxin injections, CGRP receptor antagonists, and hormone therapy such as estrogen patches or medications, can stabilize hormone levels around migraine cycles in women related to hormonal changes.
• Alternative therapies:
- Acupuncture
- Cognitive behavioral therapy or biofeedback to address psychological factors in chronic migraine


