Head Shaking or Trauma
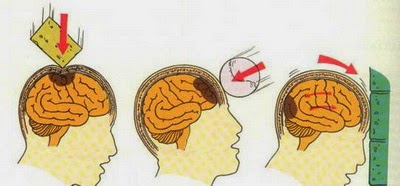
Accidentally hitting your head on a cabinet or a playful shove can cause the head to shake or be injured, which many people easily overlook. Patients often only notice discomfort 3 weeks to 3 months after the incident before seeking help from a neurosurgeon; only after an examination does the doctor find traces of impact or trauma.
Clinical analysis of over 200 brain injury patients showed that half of them had no memory at all of experiencing head shaking or trauma. Head shaking or impacts are very common in daily life. They can range from minor scalp injuries to severe loss of consciousness and life-threatening conditions.
Whether it’s a car accident or an accidental fall where you hit your head, do not assume that just because there is no bleeding or visible trauma, you don’t need a medical check-up. Intracranial hemorrhage, commonly seen clinically, involves brain trauma cases where there isn’t a single wound on the surface. If the head has experienced shaking or impact, the patient and their family must pay attention to the following:
- Whether there was a brief loss of consciousness or partial amnesia at the time of injury.
- Observe whether the injured person’s consciousness is clear; this needs to continue for at least three days.
- Whether symptoms of headache and vomiting are becoming increasingly severe.
- Whether there is numbness or weakness on one side of the arms or legs.
- Whether the walking gait is unsteady, which could indicate a cerebellar injury.
- When a brain injury patient sleeps at night, family members should monitor them closely and wake them occasionally to ensure they are conscious, preventing intracranial hemorrhage or fluid from compressing the brain and causing lethargy or coma.
Assessment and Classification of Head Trauma
The Glasgow Coma Scale (GCS) is a method used to assess a patient’s state of consciousness, with a maximum score of 15 and a minimum of 3. The scoring method is based on the patient’s Eye opening, Motor response, and Verbal response; the sum of these three is the Glasgow Coma Scale score.
Within 20 minutes after a head injury, the Glasgow Coma Scale for the patient’s consciousness is:
- (A) Mild head injury: Glasgow Coma Scale score of 13 to 15
- (B) Moderate head injury: Glasgow Coma Scale score of 9 to 12
- (C) Severe head injury: Glasgow Coma Scale score of 8 or below
Head Trauma Examination and Management
Computed Tomography (CT Scan) and Magnetic Resonance Imaging (MRI) are both widely used. CT is particularly useful as various acute intracranial hematomas, brain trauma, and cerebral edema can be clearly shown on CT images. For current head injury patients, in addition to skull X-rays, CT scans should be arranged as soon as possible for those with loss of consciousness, neurological dysfunction, or suspected intracranial hematoma.
Common Types, Symptoms, and Complications of Head Trauma:
- Scalp Hematoma:
After a head impact, a swelling often appears like an egg and is very painful. Treatment: No need for ointment, do not rub, and do not use hot compresses; it usually disappears within a month and a half. - Scalp Wound:
Attention should be paid to stopping the bleeding and keeping the wound clean. - Headache:
Headaches after head trauma vary greatly. Some people have only mild headaches, while others have unbearable pain. Some experience persistent pain, while others have intermittent pain. It can be a dull ache, a throbbing vascular pain, a burning sensation, or a feeling of pressure. The scope of the headache may be diffuse across the entire head or localized to specific areas. Changes in posture, stress, fatigue, or exertion often worsen the headache, while rest or general analgesics can provide temporary relief. - Dizziness:
Dizziness after head trauma is usually intermittent, lasting about a few minutes each time. Changing posture or psychological stress can trigger it, while lying down with eyes closed can improve it. The frequency and severity of dizziness episodes vary significantly. About half of patients with mild head injuries experience dizziness, with about half of those cases lasting more than two months. About three-quarters of patients with dizziness also have headaches, and about three-quarters of patients with headaches also experience dizziness. - Concussion:
A mild concussion refers to a situation where there is no visible head trauma, but after a heavy blow to the head, there may be a brief loss of consciousness, hearing, or smell. Other symptoms include short-term memory loss, headache, dizziness, confusion, blurred vision, unsteady gait, tinnitus, nausea, insomnia, inability to concentrate, emotional distress, or lack of energy for work. This condition should not be ignored; you should seek medical help from a neurosurgeon. If a concussion is not handled properly, it can lead to permanent sequelae. - Brain Trauma:
There is substantial damage to the brain tissue near the impact site, often involving intracranial hemorrhage. In addition to concussion-related symptoms, the severity of brain trauma can cause lethargy, coma, convulsions, limb weakness, abnormal behavior or personality changes, and rapid breathing. - Intracranial Hemorrhage (Brain Bleeding):
A hematoma directly compresses brain nerve tissue, causing damage that can lead to headaches, vomiting, rapid breathing, facial or limb convulsions, dizziness, limb weakness, numbness, changes in consciousness, lethargy, and coma. Failure to seek medical attention promptly can result in permanent disability or death. In head trauma cases, the most common fatal complications are “subdural” or “epidural” hemorrhages.- Chronic Subdural Hematoma:
If the brain trauma patient is elderly or a young child, especially those over 50, they often accidentally trip when getting up at night or fall due to an unsteady gait and hit their head. This can lead to a “chronic subdural hematoma,” which often appears slowly 2 weeks after the injury, and in some cases, up to two years later. Patients may experience headaches, one-sided weakness similar to a stroke, memory loss, or cerebellar injury causing weakness in both legs, unsteady gait, and poor appetite. However, electrolyte imbalances can also cause limb weakness, leading many elderly people to delay seeking medical treatment. Generally, the incidence of chronic subdural hematoma is low, usually about 1% to 3%, and the brain can often absorb the fluid on its own. However, if there is severe bleeding and long-term pressure on the brainstem, failure to perform minimally invasive burr hole surgery for drainage and decompression can easily lead to respiratory suppression, permanent disability, or death. - Epidural Hematoma:
This occurs when intracranial blood vessels are injured and bleed after the skull is impacted. The “dura mater” is the outermost hard tissue protecting the brain. If the bleeding is not very severe, unusual and severe headache symptoms may only appear in the first few days (averaging four to five days) after the head injury. Some patients are even misdiagnosed and treated for “migraines” or “tension headaches.” Therefore, patients with headache symptoms should inform their doctor about any history of head trauma so that an accurate differential diagnosis can be made.
- Chronic Subdural Hematoma:
- Brain Lacerations and Skull Fragments:
These directly damage tissue, and the symptoms are the same as those of brain trauma and intracranial hemorrhage. - Cerebral Edema:
After brain cells are injured, swelling (edema) often occurs, leading to central nervous system damage and potentially causing intracranial hemorrhage. - Cerebral Ischemia:
Often caused by increased intracranial pressure, leading to insufficient blood supply and resulting in brain cell damage or death. - Epilepsy:
About 2% to 7% of brain trauma patients may develop epileptic symptoms, especially those with moderate to severe brain injuries. If severe epilepsy occurs, anti-epileptic medication is required for control, and an EEG should be monitored for abnormalities.
Precautions for Head Trauma
The first 72 hours after an injury is the most critical observation period. Patients and their families must pay close attention. If the patient develops any of the following symptoms, they should contact a neurosurgeon immediately or go directly to a hospital for further examination:
- Whether there was a brief loss of consciousness or partial amnesia at the time of injury
- Severe headache or dizziness
- Lethargy or inability to be woken up (e.g., gradual loss of consciousness)
- Indifference to the outside world, inability to concentrate, or personality changes
- Loss of orientation to time and place
- Nausea, vomiting, or vertigo
- Whether there is numbness or weakness on one side of the arms or legs
- Whether the walking gait is unsteady
- When a brain injury patient sleeps at night, family members should monitor them closely and wake them occasionally to ensure they are conscious, preventing intracranial hemorrhage or fluid from compressing the brain and causing lethargy or coma


